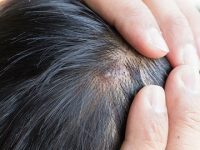
Are you tired and embarrassed of scratching your head every now and then? It could be the often overlooked condition of scalp acne, much like face acne and back acnep
Are you tired and embarrassed of scratching your head every now and then? Can’t get to the bottom of it even after treating dandruff and flaky scalp? It could be the often overlooked condition of scalp acne, much like face acne and back acne.
“Scalp acne, also known as scalp folliculitis, is a common skin condition, characterised by inflamed hair follicles on the scalp. Just like facial and body acne, scalp acne can be distressing and uncomfortable,” says consultant dermatologist Dr Manasi Shirolikar and founder of Drmanasiskin.com.
It is also a common problem faced by many in this part of the country due to the humid weather conditions. “A rise in the humidity levels creates an ideal environment for the bacteria to thrive on the scalp, leading to a higher likelihood of scalp acne outbreaks,” explains Dr Shibani Bhatia, consultant dermatologist at Kaya Clinic, Mumbai.
Giving more details on the condition, the experts decode how to deal with scalp acne, which can manifest in various forms, each with distinct characteristics. Here are the different types of scalp acne.
- Papules and pustules: These are small, raised bumps on the scalp, similar to facial acne.
- Scalp abscesses: Deeper and more painful than papules and pustules, these are often filled with pus.
- Scalp folliculitis: Characterised by redness and itching, this type of scalp acne can sometimes lead to hair loss.
TREAT IT RIGHT
Medicated shampoos: Look for shampoos that contain ingredients like salicylic acid, ketoconazole or selenium sulfide, which help control oil production, combat fungal and bacterial infections.
Gentle cleansing: Avoid vigorously scrubbing your scalp during hair washes as it can worsen inflammation. Instead, gently massage the scalp.
Check products: Look for any existing products such as oils, dry shampoos or any new products that could have led to scalp folliculitis.
Prescription medications: For severe cases, dermats may prescribe topical or oral antibiotics, antifungal medicines or corticosteroids.
WAYS TO FIX IT AT HOME
Oil your hair: If you’re prone to scalp folliculitis, remember to apply oil on your scalp and not hair. Also, ensure you don’t leave it on for more than an hour before washing.
Regular scalp washes: It is advised to wash your hair with a gentle, sulphate-free shampoo, more importantly when your scalp feels oily and greasy.
Warm compress: Applying a warm, damp cloth to the affected areas can reduce pain and inflammation.
KEEP ACNE AT BAY
Regular shampooing: Wash your hair regularly, especially after sweating and working out to remove excess oil and prevent build-up of dirt and dead skin cells.
Avoid hair products: Some hair products such as heavy conditioners and styling gels, can cause acne.
Dietary considerations: Although there is limited scientific evidence, some people find that reducing dairy and high-glycemic foods may help improve scalp acne.
Avoid oil-based products: Opt for non-comedogenic hair care products to prevent clogged follicles.
WHAT CAUSES IT?
Excessive oil production: Overproduction of sebum (skin oil) can clog hair follicles, leading to acne.
Dead skin cells: When dead skin cells mix with oil, they can block hair follicles and promote acne.
Bacterial infection: Bacteria, especially Propionibacterium acnes (P acnes) and Staphylococcus Aureus can infect hair follicles and cause inflammation.
Fungal infection: Yeast or fungi, such as Malassezia, can contribute to scalp acne.
Not washing hair often: Excessive sweating can trap sweat and bacteria in hair follicles and skipping hair washes can lead to acne.
Wrong products: Using products like heavy oils, pomades or wax can clog hair follicles. Hair products that have alcohol can further cause irritation of the scalp leading to more oil production.
https://www.hindustantimes.com/lifestyle/fashion/tired-of-itchy-acne-on-your-scalp-here-s-what-can-help-101697538162097.html