Introduction
Many survivors experience long-term symptoms for months after the clinical resolution of the viral infection. This is termed post-acute sequelae of COVID-19 (PASC) or long Covid.
Six mechanisms have been proposed for long COVID symptoms, which include the persistence of SARS-CoV-2, hyperactivation of platelets and the formation of microclots, autoantibody formation, dysregulated immunity, multi-organ dysfunction, and reactivation of SARS-CoV-2 from dormancy.
A new study published on the preprint server medRxiv* determines how endothelial activation and inflammation contribute to the formation of microclots in PASC.
Platelet activation and fibrinaloid microclots
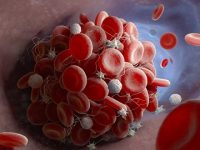
Earlier reports have described the presence of microclots in the circulation of patients with long Covid. These microclots, which resist normal clot breakdown by fibrinolysis, are composed of fibrin amyloid and can result from plasma activation by the SARS-CoV-2 spike protein.
Within these microclots lies an array of trapped inflammatory chemicals such as alpha 2-antiplasmin (α2AP), various fibrinogen chains, von Willebrand factor (vWF), platelet factor 4 (PF4), serum amyloid A (SAA), and various antibodies. Thus, acute coagulopathy characterizes acute severe COVID-19.
Without resolving this process, persistent and toxic hypoxia and poor oxygen exchange at the tissue level may cause lingering damage. A recent report showed a higher-than-expected incidence of clots and other vascular events for up to 49 weeks from the onset of the acute infection.
About the study
The current study identifies markers in the soluble fraction of blood, as opposed to the solid components, that could help confirm the role of endothelial pathology and coagulopathy in long COVID.
Biomarkers were selected from earlier reports in which they were described as being trapped within the microclots and included vWF, PF4, SAA, and α-2AP. In addition, endothelial injury markers, including endothelial-leukocyte adhesion molecule 1 (E-selectin) and platelet endothelial cell adhesion molecule1 (PECAM-1), were also analyzed.
Each of these molecules is released during endothelial activation or abnormal activation of coagulation pathways. Some, like α-2AP, impair fibrinolysis, thus allowing microvascular thrombosis to occur around the abnormal clots and increasing the risk of thromboembolism. This molecule is already a predictive marker of poor outcomes in patients with cardiovascular disease.
The markers of endothelial dysfunction were chosen because of the central role of this phenomenon in long COVID. In addition to looking for increases in these compounds in long COVID, the scientists examined their participation in protein-protein interactions with plasma proteins to trigger microclot formation and with platelet receptors to cause platelet hyperactivation.
What did the study show?
All six molecules were present at higher mean levels in patients with long COVID compared to others, thus corroborating earlier research.
Specifically, α-2AP levels rose above upper normal limits, with increased mean levels of the other five molecules in samples from long COVID patients compared to controls. The actual levels are likely to be much higher, the researchers suggest.
These molecules mediate inflammation and platelet activation, triggering endothelial damage and extensive vascular injury. The current study added to this knowledge by showing how their concentrations in the soluble fraction of plasma were raised in long COVID patients.
The six markers are involved in various coagulation processes. For example, vWF triggers intravascular platelet activation and aggregation, thus leading to thrombosis due to fibrinogen binding. In addition, SAA binds to several extracellular matrix molecules and endothelial toll-like receptors (TLRs), subsequently contributing to the release of inflammatory mediators and reactive oxygen species (ROS).
The resulting injury to the endothelium is linked to functional impairment of this tissue and early atheroma formation. This process also activates the NLRP3 inflammasome, then causing thrombin production by activating the coagulation cascade.
Increased levels of α-2AP cause microclots to resist fibrinolysis by binding to plasmin, which has fibrinolytic properties. This causes clots to develop in arteries and veins, embolism, and ischemic stroke.
The increased levels of E-selectin also confirm endothelial activation. This molecule tethers white blood cells to endothelial cells, allowing them to roll on activated endothelium and ultimately triggering platelet-endothelium adhesion.
E-selectin and PECAM-1 were reported to cause microclots and platelet hyperactivation in blood samples from healthy patients, which was similarly reported in previous samples obtained from long COVID patients. These events could be due to protein-protein interactions with plasma proteins that cause misfolding and platelet receptors that lead to hyperactivation.
Conclusions
Impaired coagulation that contributes to ischemia-reperfusion injury due to the formation of fibrinolysis-resistant fibrin-amyloid microclots is a key mechanism responsible for developing long COVID. This is supported by the presence of such clots and relatively elevated levels of six inflammatory mediators that play vital roles in coagulation and endothelial activation.
https://www.news-medical.net/news/20221018/New-research-finds-microclotting-and-inflammatory-molecule-abnormalities-in-long-COVID.aspx